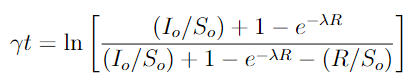Imagine you're an athlete playing your favorite sport. Your moment in the big game has come and the outcome now entirely hinges on your ability to reach deep and put out your peak performance. What does that mean for you?
If you are an athlete in excellent shape after years of conditioning with the daily support of the world's best trainers, you probably have a good idea of what your maximum effort can produce. But what if you're not and you find yourself in a situation where your athletic ability will be put to the test? Such a moment might come in the form of a friendly pickup game or just playing with your kids. Or it could come because you need to make a mad dash to catch your connecting flight at the airport before the gate closes. In all these situations, your fitness matters, so how fit are you really?
Most people don't have access to the top trainers and the equipment they use to bring professional athletes to the highest level of their performance. You may be surprised to learn you don't necessarily need that access to get a relatively good idea of how fit you really are.
What you need is an estimate of your VO₂ max, which according to Harvard Health, is "an objective measurement to tell just how fit you are". Here's how they describe the metric:
The V in VO₂ max stands for volume, while O₂ max stands for oxygen. As such, VO₂ max measures how much oxygen your body consumes while exercising. Typically, VO₂ max is measured as ml/kg/minute (milliliters of oxygen consumed per kilogram of body weight per minute of exercise).
When you breathe, your lungs absorb oxygen and transport it your red blood cells, which carry the oxygen to all of your body's organs and muscles. Your muscle cells need oxygen to generate adenosine triphosphate (ATP). ATP provides the main energy source your muscles need to do their work. The more oxygen you can breathe in, the more ATP your muscles produce, creating the energy to fuel your muscles and power your workout. (This is also why you breathe faster while exercising.)
If you have a higher VO₂ max, that means your heart and lungs are more effectively supplying blood to your muscles, and that your muscles are efficiently extracting and using oxygen from your blood. That's why a high VO₂ max is a good indicator of a high fitness level.
How high is your VO₂ max?
If you know a professional trainer who has access to an exercise medicine lab, they can hook you up to an apparatus that measures how much air you breathe while you engage in intense physical activity to get the best possible estimate of your VO₂ max. If you're like most of us, you don't have that access, but that's not a limitation.
That's because you can get a reasonable estimate of your VO₂ max by taking a very brisk walk on a relatively flat, mile-long path, a stopwatch, and a calculator. It wouldn't hurt to have a smart watch or other device that can measure your heart rate, but if you know how to take your pulse, you can get by with just a stopwatch or even a regular watch with a second hand.
What you'll do with those things is take the One-Mile Rockport Walking Test:
The one-mile walking test is an evaluation of cardiovascular fitness, that seeks to predict an individual’s aerobic capacity, which is also known as VO₂ max, or maximal oxygen consumption.
The one-mile walking test was developed by researchers in 1986 as an alternative assessment to accurately predict an individual’s aerobic capacity following a one-mile track walk. The test is both indirect and sub-maximal in nature, making it considerably easier to implement in field-based scenarios. While the test should be completed on a track or suitably flat terrain, it could reasonably be replicated on a treadmill.
The one-mile walking test is designed for both men and women aged 20-69 of varying levels of fitness. As the test only requires a participant to perform a brisk walk, it is also suitable for deconditioned participants, older adults, or those that are overweight.
Research conducted in 2011 found the one-mile walk test to be a valid predictor of VO2 max and a reliable alternative to the 1.5-mile run test that is widely used by the military.
Pretty impressive, right? HFE gives the following instructions to do it, which we've given a minor tweak:
- If available, attach the heart rate monitor and ensure that it is correctly measuring heart rate
- Start the stopwatch and commence walking
- Walk the planned route as quickly as possible without running or skipping
- Ensure that throughout the test, there is always 1-foot on the ground
- On completion of the distance, stop the clock and record the heart rate immediately
Our minor tweak is to the first step, where we added the words "if available". If you don't have a heart rate monitor available, take your pulse for fifteen seconds after completing the distance. You can then find your heart rate by multiplying the beats you count by four, which will determine your heart's beats-per-minute.
From here, you'll take your "as quick as possible" walking time for the mile, your heart's beats per minute at the end, your sex, your weight (in pounds), and your age and enter them in the following tool we built to use this information in a formula that will estimate your VO2 max. We've set the following tool up with some default data, please substitute your own data to get your results. If you're accessing this article on a site that republishes our RSS news feed, you may need to click through to our site to access a working version of the tool.
Once you have your results, compare them with the information in the following tables, which are also available at HFE's site:
The default data in the tool gives a VO₂ max value of 48.03 for our hypothetical 30-year-old, 180-pound man who walked one mile in 12 mintues and 15 seconds while their heart rate at the end clocked in at 164 beats per minute (which is what you would enter in the tool if you took your pulse for 15 seconds at the end of the walk, counted 41 beats, then multiplied this figure by four). According to the tables, our fast-walking test taker would be considered to be average in cardiovascular fitness for their age group (Age 21-30) and sex.
Remember to substitute your own data! Afterward, you will have a much better idea of how fit you really are. Best of all, you didn't have to strap on any strange breathing apparatus while hooked up to monitoring machines that go "beep"!
Update Bonus video!
HT: ACSH.
Image Credit: Person in white and black nike shoes photo by Sincerely Media on Unsplash.
Health care professionals have a new tool in their medical kits for assessing the health of their patients. The Body Roundness Index has the promise of overcoming several of the weaknesses of the long-established Body Mass Index (BMI), which has often been misused as a health indicator by the profession.
BMI has become entrenched in large part because it has two basic inputs that are easy to measure: height and weight. These two factors are combined in a mathematical formula to provide a single value to indicate how relatively healthy an individual is based on just their weight and height. Or would if it were used appropriately.
Like BMI, the Body Roundness Index (BRI) has simple inputs that can be easily obtained using standard height gauges and measuring tapes: height and waist circumference. The Conversation describes how it came about and its potential:
BRI was developed by US researchers in 2013 in response to criticisms of BMI. Instead of looking at height and weight, BRI mathematically quantifies body fat levels by looking at height and waist circumference instead. This provides a value typically ranging from one to 20. It is the lowest and highest values that suggest the highest health risk.
Numerous studies have shown that BRI may be better than BMI at predicting the health risks associated with different levels of body fat. This includes predicting risk of weight-related diseases such as cardiovascular disease, diabetes, kidney disease and cancer, as well as death from any cause.
This latest study, which looked at 32,995 US adults between 1999 and 2018, found an association between BRI and death from any cause. Specifically, they also found that people with the lowest and highest BRI scores had the greatest health risks.
They also found that BRI was better than BMI at accurately detecting this risk. This is because BRI considers the fat held around the abdomen, which is linked to greater risk of health problems. This is different to BMI, which only considers overall weight.
BRI has the potential to be a better indicator of an individual's relative health than BMI while also being far less expensive, especially when compared with the alternative of today's more exact medical scanning and sensing technologies. And while's there's an online tool that can calculate your BRI, it's a little clunky to use. Especially if you want to run a number of "what if" scenarios in short order, like you would if you wanted to find out where it sets the boundary between being in or out of what it identifies as "the healthy zone" for someone of your height.
Which is to say we think there's room in the tool marketplace for a simpler, more bare bones tool to do the math. So we built it. Just enter the indicated measurements and the tool will do the math. If you're accessing this article on a site that republishes our RSS news feed, please click through to our site to access a working version.
As you can see, our tool is as bare bones as it gets. As a bonus, because of the underlying math, we don't have to worry about the units of measurement, provided they are the same. Use inches for both your height and waist circumference, you're good to go. The same is true if you use centimeters for both. Or cubits, if you must. The only limitation is you can't mix and match units and expect to get reliable results.
Now that you have the result for what you entered, what might it tell you?
That's where the long term study of Americans' health comes into play. The following chart presents all-cause mortality based on BRI for the individuals included in the study from 1999 through 2019. Find your BRI on the horizontal axis, then look up to see where the U-shaped curve puts your relative risk of death compared to where the minimum risk is at the lowest point of the curve.
In this chart, the solid blue curved line is the estimate of all-cause mortality for individuals with the Body Roundess Index indicated in the horizontal axis, and the light blue shading represents the 95% confidence interval for each level.
Here's what the authors have to say about what the chart shows:
As an extension, we expanded NHANES cycles from 1999 through 2018 and followed up to December 31, 2019, and we observed a U-shaped risk trajectory for the association between BRI and all-cause mortality. Differing from the study by Zhou et al, we chose the middle quantile (BRI, 4.5-5.5) of this U-shaped trajectory as the reference and found that all-cause mortality risk was increased by 25% for adults with BRI less than 3.4 and by nearly 50% for adults with BRI 6.9 or greater. The magnitude of risk estimation persisted even after excluding accidental deaths or deaths within 2 years or reserving participants with myocardial infarction, stroke, congestive heart failure, or cancer. Hence, estimates of mortality risk associated with BRI may help inform decision-making in clinical settings.
In this national cohort, we noticed that very low BRI was associated with a significantly increased risk of all-cause mortality, especially in individuals aged 65 years and older. This association seems plausible, as BRI was identified as a potential proxy measure associated with nutritional status, and very low BRI can be accompanied with malnutrition, fatigue, reduced activity tolerance, and muscle atrophy. The reasons behind the association between BRI and mortality may be epidemiologically and clinically plausible. From epidemiological aspects, elevated BRI was significantly associated with an increased risk of cardiovascular and metabolic disorders, and even cancer, which might serve as the culprits responsible for all-cause mortality. From clinical aspects, the accumulation of visceral fat was associated with more profound insulin resistance and an increased risk of cardiometabolic diseases, even among participants with weight within reference range.
Aside from its potential as a better-than-BMI health indicator, BRI also caught our attention because the math behind incorporates the formula for the eccentricity of an ellipse. Which you can see if you look closely at our AI-generated version of DaVinci's Vitruvian Man sketch.
References
Zhang X, Ma N, Lin Q, et al. Body Roundness Index and All-Cause Mortality Among US Adults. JAMA Netw Open. 2024;7(6):e2415051. DOI: 10.1001/jamanetworkopen.2024.15051.
Thomas, DM; Bredlau, C; Bosy-Westphal, A; et al. Relationships between body roundness with body fat and visceral adipose tissue emerging from a new geometrical model. Obesity (Silver Spring). 2013;21(11):2264-2271. DOI: 10.1002/oby.20408.
Image Credit: Microsoft Copilot Designer.. Prompt: "Vitruvian Man with an ellipse as long as the man is tall and as wide as the man's waist".
Life expectancy in the United States has started to recover after taking a big hit from 2020's Coronavirus Pandemic.
That's the big story following the CDC's release of its provisional life expectancy estimates for 2022 at the end of November 2023. After peaking at 78.8 years in 2019 (76.3 years for males and 81.4 years for females), average American life expectancy at birth dropped during 2020 and 2021, bottoming at 76.4 years (73.5 years for males and 79.3 years for females).
But in 2022, it began to rebound. Average life expectancy at birth rose to 77.5 years, with life expectancy rising by 1.3 years to 74.8 years for males and rising by 0.9 years to 80.2 years for females. The CDC finds "declines in mortality due to COVID-19 were the primary reason for the increases in life expectancy from 2021 to 2022 observed for the total population".
The following chart showing how life expectancy from birth has changed for Americans from 2000 through 2022 is taken from the CDC's report presenting its provisional findings for 2022.
While the decline in COVID-19 mortality led the improvement in U.S. life expectancy, it wasn't the only contributor to it.
The increase of 1.1 years in life expectancy from 2021 to 2022 primarily resulted from decreases in mortality due to COVID-19 (84.2% of the positive contribution), heart disease (3.6%), unintentional injuries (2.6%), cancer (2.2%), and homicide (1.5%) (Figure 4). The increase in life expectancy would have been even greater if not for the offsetting effects of increases in mortality due to influenza and pneumonia (25.5%), perinatal conditions (21.5%), kidney disease (13.0%), nutritional deficiencies (12.6%), and congenital malformations (5.9%).
The CDC's provisional data for 2022 will be finalized over the next months as the agency is still accumulating death certificate data.
References
Arias, Elizabeth; Kochanek, Kenneth D.; Xu, Jiaquan; Tejada-Vera, Betzaida. Provisional Life Expectancy Estimates for 2022. National Center for Health Statistics (U.S.). VSRR; no 31. [PDF Document]. 29 November 2023.
NAMES. United States Life Tables, 2019. National Center for Health Statistics (U.S.). National Vital Statistics Reports, Vol. 70, No. 19. [PDF Document]. 22 March 2022.
Image credit: Human development stages (collage) on Wikimedia Commons. Creative Commons. CC BY-SA 3.0 DEED Attribution-ShareAlike 3.0 Unported.
Labels: health
How different would New York City's experience during the first wave of 2020's coronavirus pandemic have been if public officials had better and more timely information about how many people were really being infected by it?
That's a fascinating question raised by the Empire Center's Bill Hammond's retrospective analysis of the pandemic's impact in New York. In that analysis, Hammond features a chart comparing the information public officials had on the number of confirmed COVID-19 cases with the Institute for Health Metrics and Evaluation's improved estimates of how extensive coronavirus infections likely were in reality in early 2020. Here's a slightly modified* interactive version of the chart:
Compared with the official count produced by the New York State Department of Health (NYSDOH) in early 2020, COVID-19 infections were much more numerous and peaked much earlier in the IHME's improved estimates Hammond describes what the chart shows:
As seen in Figure 1, the state’s outbreak likely began by early February, a full month before its first laboratory-confirmed case [2]. The estimated number of infections soared to more than 60,000 per day on March 19, which was six times higher and three weeks earlier than shown by the state’s testing data.
A second attempt to model the first wave of New York’s pandemic estimated that it began on Jan. 19 and reached a peak infection rate of almost 100,000 per day on March 24 [3]. These estimates indicate that the curve had already begun to bend – that is, the rate of increase had begun to slow – before Cuomo issued his stay-at-home order effective March 22 – likely because individuals and businesses were spontaneously limiting their activities in reaction to official warnings and news coverage.
Hammond explains how better knowledge of the true picture for the spread of COVID-19 infections could have shaped the response of both New York's governor and the state's public health officials:
The virus’s rapid spread in February and early March of 2020 shows the importance of detecting outbreaks early and responding quickly. If officials had become aware of this surge even a week or two sooner – and notified the public – they almost certainly could have avoided swamping hospitals and saved thousands of lives.
If they had merely known when the wave reached its peak, they might have avoided mistakes in late March.
For example, Cuomo and his administration would have had less cause to worry about a looming shortage of hospital capacity. They could have avoided spending time and money to build emergency hospital facilities that went largely unused. And they might never have issued the March 25 directive transferring Covid-positive patients into nursing homes – a decision that likely added to the high death rate in those facilities and contributed to Cuomo’s political downfall. [6]
Here's an example of the official data and modeled projections they did have in early 2020. The following chart is taken from the Institute for Health Metrics and Evaluation (IHME)'s 25 March 2020 projections showing its estimates of the minimum, likely, and maximum number of additional hospital beds that would be needed in the state of New York to care for the model's expected surge of coronavirus patients.
This chart presents just one of several coronavirus models whose projections were being combined and presented to Governor Cuomo by consultants from McKinsey & Co. to assist their ad hoc public health policy making. Had New York state government officials instead known the daily number of new COVID-19 infections had already passed its peak, they almost certainly would not have reached the point of panic they did. Panic that resulted in their creating one of the worse public health outcomes in U.S. history.
Unlike those now mostly-former New York state officials, the IHME is at least learning from its mistakes in modeling 2020's coronavirus pandemic.
Previously on Political Calculations
References
Hammond, Bill. Behind the Curve: The Extreme Severity of New York City's First Pandemic Wave. Empire Center. [PDF Document]. 30 August 2023.
Institute for Health Metrics and Evaluation. COVID-19 estimate downloads. March 25, 2020. [ZIP folder]. Accessed 15 October 2023.
Footnotes from Behind the Curve
[2] https://www.healthdata.org/covid/data-downloads.
[3] David García-García et al., “Identification of the first COVID-19 infections in the US using a retrospective analysis (REMEDID),” Spatial and Spatio-temporal Epidemiology, Vol. 42, August 2022. https://www.sciencedirect.com/science/article/pii/ S1877584522000405#fig0001.
[6] For more on the Cuomo administration’s handling of the pandemic in nursing homes, see the Empire Center’s August 2021 report, “ ‘Like Fire Through Dry Grass’: Documenting the Cuomo Administration’s Cover-up of a Nursing Home Nightmare.” https://www.empirecenter.org/publications/like-fire-through-dry-grass/
Other Notes
* We altered the dimensions of the chart and the line thickness for the IHME estimate of infections. We also added the options for downloading a copy of the chart and sharing it on social media.
Labels: data visualization, health, risk
Early during the coronavirus pandemic, researchers in many fields got a crash course in epidemiology. More specifically, they got a crash course in how to apply the math behind the SIR model, which describes how fast a contagious condition might spread through a population before becoming endemic.
The SIR model divides a population into three categories, the Susceptible, the Infectious, and the Recovered (or Removed). Once basic data about the rates of infection and recovery are determined, the model can simulate how many people will fall within each of these categories at different points of time. Here's a primer introducing that basic math, in which we featured the following 22-minute video from Numberphile's Brady Haran and Ben Sparks on how to build your own SIR model from scratch using the online GeoGebra application:
Although each of the individual equations for each component of the SIR model involves relatively simple relationships, their interactions lead to much more complex math. Math that cannot be done simply by plugging numbers into an algebraic formula. Instead, the SIR model's math requires serious computing power to apply numerical methods, running thousands or millions of calculations to progressively reach reasonably accurate, but still not exact solutions.
That's why the press release for a paper recently published in the International Journal of Chemical Kinetics caught our attention. Its authors recognized part of the SIR model's math developed by epidemiologial pioneers W. O. Kermack and A. G. McKendrick is identical to the math used to describe the progress of an autocatalytic reaction in chemistry. Here's the Kermack-McKendrick integral, which has no direct solution:
In this equation, So and Io represent initial values for the number of Susceptible and Infectious portions of the popuation, R represents the Recovered (or Removed) portion of the population as a function of time (t), while the Greek letter lambda (λ) represents the ratio of the rate of spread among susceptible population to the rate of recovery. The letter e is Euler's constant.
That was math for which chemists James Baird, Douglas Barlow and Buddhi Pantha had developed the next best thing to a direct solution. They derived an approximate algebraic formula for quickly solving the Kermack-McKendrick integral with a small margin of error. Here's their simplified formulation:
Better still, they identified where their simplified formulation will work best:
In this report, a description is given of an accurate approximation to the Kermack-McKendrick integral which in turn can be used to determine values for R(t), I(t) and S(t) in the SIR epidemic model. The result is shown to be effective for situations where 1.5 ≤ Ro ≤ 10 with no need to numerically compute an integral.
The press release better describes how their formulation meshes with the chemistry of autocatalytic reactions:
Dr. Baird presented the model in May at the Southeastern Theoretical Chemistry Association meeting in Atlanta.
"The World Health Organization could program our equation into a hand-held computer," Dr. Baird says. "Our formula is able to predict the time required for the number of infected individuals to achieve its maximum. In the chemical analog, this is known as the induction time."
The formula is capable of predicting the number of hospitalizations, death rates, community exposure rates and related variables. It also calculates the populations of susceptible, infectious and recovered individuals, and predicts a clean separation between the period of onset of the disease and the period of subsidence....
"The rate of infection initially accelerates until it reaches a point where the infection rate is balanced by the recovery rate of infected individuals, at which point the number of infected people peaks and then starts to decay," he says.
That mechanism reminded him of the mechanism that governs an autocatalytic reaction.
"I subsequently learned that the mathematical description of the spread of infectious diseases was first described by Kermack and McKendrick," Dr. Baird says.
"When I read their paper, I realized that their mechanism was exactly the same as that of an autocatalytic reaction, where a catalyst molecule combines with a reactant molecule to produce two catalyst molecules," he says. "The rate of production of catalyst molecules accelerates until it is balanced by the rate of decay of the catalyst to form the product."
And that's how the algebraic formula that can quickly approximate the solution to the Kermack-McKendrick integral for the epidemiological SIR model with minimal computing power came to be published in a chemistry journal.
References
James K. Baird et al, Analytic solution to the rate law for a fundamental autocatalytic reaction mechanism operating in the "efficient" regime, International Journal of Chemical Kinetics (2022). DOI: 10.1002/kin.21598.
James K. Baird, Douglas A. Barlow, Buddhi Pantha. A Solution for the Principle Integral of the Kermack-McKenrick Epidemiological Model. [Preprint (PDF)]. DOI: 10.31224/2264. April 2022. [This second paper is an ungated preprint that focuses on the epidemiological application of the authors' approximation of the Kermack-McKendrick integral.]
How much health risk do you have from carrying too much mass around your midsection?
That question arises because studies point to the Waist-to-Height Ratio (WHtR) as a better indicator of early health risk than the Body Mass Index (BMI). As a general rule of thumb, if the circumference of your waist is greater than half your height, you have an elevated risk for developing chronic conditions like hypertension, diabetes mellitus, hypercholesterolemia, joint and low back pains, hyperuricemia, and obstructive sleep apnea syndrome.
The Waist-to-Height Ratio is also reported to be better than BMI in predicting heart attacks, especially for women, with higher ratios corresponding to higher risk.
That sounds like good bit of information to have, so we've built a tool to calculate your Waist-to-Health Ratio. Since you probably already know your height, the hard part will be finding out your waist circumference. Here's a video showing how to measure it.
Once you've done that for yourself, you're ready to go. If you're accessing this article on a site that republishes our RSS news feed, please click through to our site to access a working version of the tool. Here it is:
In using the tool, be sure to use the same units of measurement for both waist circumference and height. You'll get accurate results so long as you don't start mixing and matching inches and centimeters together....
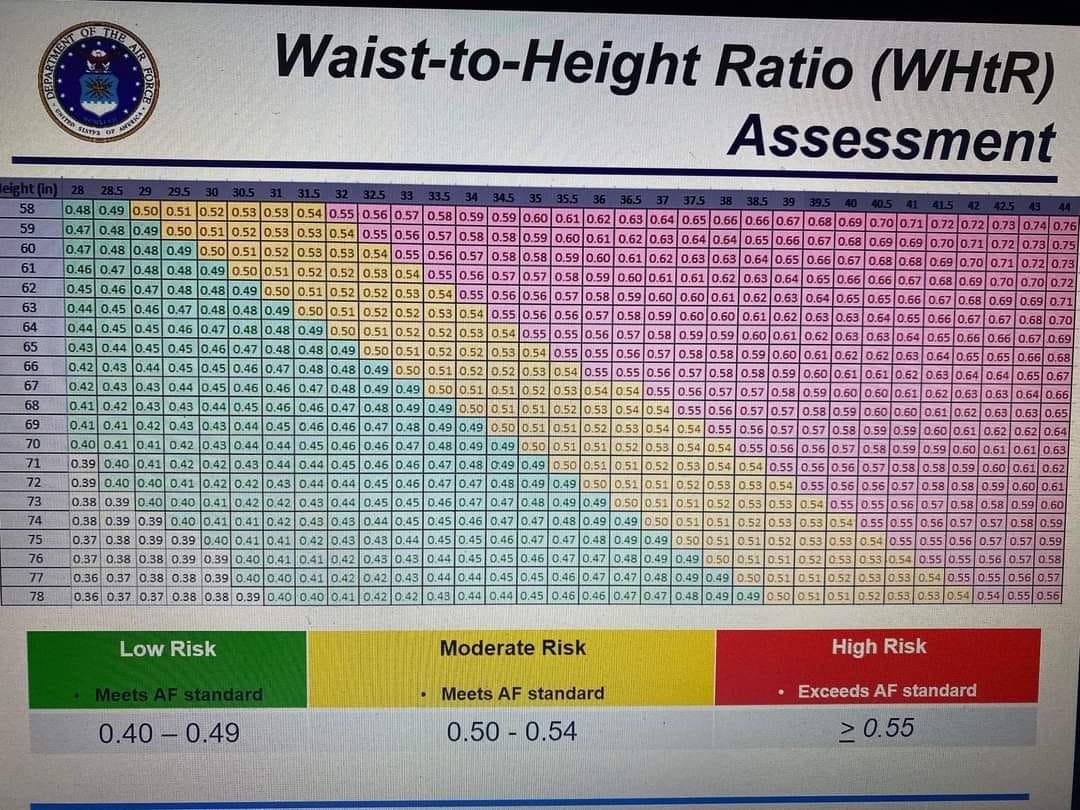
According to documents leaked in February 2022, starting in July 2022, U.S. Air Force personnel will have their Waist to Height Ratio assessed. Individuals with waists that measure at more than half their height will be reassessed six months later, with those whose waists exceed that threshold at the later measurement date separated from service. "Seperated from service" meaning "discharged from the Air Force". Here's the chart the Air Force will be using to make that determination:
The thresholds shown on this chart for low, moderate, and high risk are those we've built into the tool's feedback. We've also made a point of giving the answer to the same two-decimal place results as would be used by Air Force medical personnel in their assessments, so there are no surprises for what to expect.
Previously on Political Calculations
References
Margaret Ashwell and Sigrid Gibson. Waist-to-height ratio as an indicator of ‘early health risk’: simpler and more predictive than using a ‘matrix’ based on BMI and waist circumference. BMJ Open 2016:6:3010159. [DOI: 10.1136/bmjopen-2015-010159 | NIH: PDF Document]. 14 March 2016.
Sanne A.E. Peters, Sophie H. Bots and Mark Woodward. Sex Differences in the Association Between Measures of General and Central Adiposity and the Risk of Myocardial Infarction: Results From the UK Biobank. Journal of the American Heart Association. Vol. 7, No. 5. [DOI: 10.1161/JAHA.117.008507]. 28 February 2018. American Heart Association. Waist size predicts heart attacks better than BMI, especially in women. [Online Article]. 28 February 2018.
Darsini Darsini, Hamidah Hamidah, Hari Basuki Notobroto, and Eko Agus Cahyono. Health risks associated with high waist circumference: A systematic review. Journal of Public Health Research. Vol. 9, No. 2: Papers from the 4th International Symposium of Public Health (4th ISOPH), Brisbane, Australia. 29-31 October 2019. [DOI: 10.4081/jphr.2020.1811 | NIH: PDF Document]. 2 July 2020.
ShapeFit. Waist to Height Ratio Calculator - Assess Your Lifestyle Risk. [Online Article and Tool]. 31 March 2015.
Imagine this scenario. Public health advocates campaign for your city to impose a tax on sugary beverages. They claim it will improve the public's health through fighting obesity by making soda and other soft drinks made with sugar more costly to buy, forcing budget-minded consumers to substitute much lower calorie containing beverages. Your city's politicians, always happy to get more tax revenue, go along with their scheme. How do you think consumers of sugary soft drinks in your city will respond?
If you answered they will drink more calorie-laden alcohol-based beverages, you're right!
The latest proof that consumers substitute beer and liquor for sugar-sweetened soft drinks comes to us from Seattle. In December 2017, the city imposed a unique $0.0175 per ounce tax on beverages containing calories from sugar, but not on beverages made with non-calorie-laden sweeteners. For example, consumers buying a two-liter bottle of Coca-Cola would pay an additional tax of $0.35 that consumers of the same size bottle of Diet Coke or Coke Zero would not.
At first glance, you might think consumers of Sugar-Sweetened Beverages (SSB) would choose to switch to the sugar-free versions of their previously preferred soft drink or to water to avoid having to pay so much more for it.
But that's not what happened according to a peer-reviewed study published in PLOS ONE, which found that the tax "induces substitution to alcoholic beverages". More specifically, the consumers preferred substitute wasn't sugar-free beverages. It was beer, whose sales rose by 7% relative to those of the demographically similar city of Portland, Oregon, which didn't impose a soda tax:
There was evidence of substitution to beer following the implementation of the Seattle SSB tax. Continued monitoring of potential unintended outcomes related to the implementation of SSB taxes is needed in future tax evaluations.
How many competent public health advocates do you suppose would push for new or expanded soda taxes knowing that real life consumers are more likely to shift to alcohol-based beverages with equivalent levels of calories instead of water or low-calorie sugar-free soft drinks? Not only do they miss any benefit from reducing calories consumed among the public, higher alcohol consumption comes with the "higher risk of motor accidents/deaths, liver cirrhosis, sexually transmitted diseases, crime and violence, and workplace accidents" to the public's health.
Then again, if you're a long-time reader of Political Calculations, you could have easily predicted that from our analysis of what happened to alcohol sales in Philadelphia after that city's soda tax went into effect.
Image credits: Coca-Cola Photo by Omar Elmokhtar Menazeli on Unsplash. Miller High Life Photo by Waz Lght on Unsplash.
References
Lisa M. Powell, Julien Leider. Impact of the Seattle Sweetened Beverage Tax on substitution to alcoholic beverages. PLOS ONE 18 January 2022. DOI: 10.1371/journal.pone.0262578.
Baylen Linnekin. Study: Seattle's Soda Tax Has Been Great for... Beer Sales? Reason. [Online Article]. 12 February 2022.
Previously on Political Calculations
The reports of how COVID-19 changed U.S. life expectancy are grim.
The pandemic crushed life expectancy in the United States last year by 1.5 years, the largest drop since World War II, according to new Centers for Disease Control and Prevention data released Wednesday. For Black and Hispanic people, their life expectancy declined by three years.
U.S. life expectancy declined from 78.8 years in 2019 to 77.3 years in 2020. The pandemic was responsible for close to 74 percent of that overall decline, though increased fatal drug overdoses and homicides also contributed.
“I myself had never seen a change this big except in the history books,” Elizabeth Arias, a demographer at the CDC and lead author of the new report, told The Wall Street Journal.
The figures for just COVID-19's impact on U.S. life expectancy are roughly in line with the CDC's preliminary estimates from February 2021, which was based on the then-available data through the first half of 2020.
Unfortunately, the CDC's estimates are rather misleading. Dr. Peter Bach, the director of the Center for Health Policy and Outcomes at the Memorial Sloan Kettering Cancer Center, ran some back of the envelope calculations after the CDC released its preliminary estimates and came up with very different results.
The CDC reported that life expectancy in the U.S. declined by one year in 2020. People understood this to mean that Covid-19 had shaved off a year from how long each of us will live on average. That is, after all, how people tend to think of life expectancy. The New York Times characterized the report as “the first full picture of the pandemic’s effect on American expected life spans.”
But wait. Analysts estimate that, on average, a death from Covid-19 robs its victim of around 12 years of life. Approximately 400,000 Americans died Covid-19 in 2020, meaning about 4.8 million years of life collectively vanished. Spread that ghastly number across the U.S. population of 330 million and it comes out to 0.014 years of life lost per person. That’s 5.3 days. There were other excess deaths in 2020, so maybe the answer is seven days lost per person.
No matter how you look at it, the result is a far cry from what the CDC announced.
We built the following tool to do Bach's math, which checks out. You're welcome to update the figures with improved data or to replace them with other countries' data if you want to see the impact elsewhere in the world. If you're accessing this article on a site that republishes our RSS news feed, please click through to our site to access a working version of the tool.
So why is the CDC's estimate of the change in life expectancy estimate so different? As Bach explains, it is not because of either the data or the math, but rather, it is because of the CDC's assumptions in doing their math:
It’s not that the agency made a math mistake. I checked the calculations myself, and even went over them with one of the CDC analysts. The error was more problematic in my view: The CDC relied on an assumption it had to know was wrong.
The CDC’s life expectancy calculations are, in fact, life expectancy projections (the technical term for the measure is period life expectancy). The calculation is based on a crucial assumption: that for the year you are studying (2019 compared to 2020 in this case) the risk of death, in every age group, will stay as it was in that year for everyone born during it.
So to project the life expectancy of people born in 2020, the CDC assumed that newborns will face the risk of dying that newborns did in 2020. Then when they turn 1, they face the risk of dying that 1-year-olds did in 2020. Then on to them being 2 years old, and so on.
Locking people into 2020 for their entire life spans, from birth to death, may sound like the plot of a dystopian reboot of “Groundhog Day.” But that’s the calculation. The results: The CDC’s report boils down to a finding that bears no relation to any realistic scenario. Running the 2020 gauntlet for an entire life results in living one year less on average than running that same gauntlet in 2019.
Don’t blame the method. It’s a standard one that over time has been a highly useful way of understanding how our efforts in public health have succeeded or fallen short. Because it is a projection, it can (and should) serve as an early warning of how people in our society will do in the future if we do nothing different from today.
But in this case, the CDC should assume, as do we all, that Covid-19 will cause an increase in mortality for only a brief period relative to the span of a normal lifetime. If you assume the Covid-19 risk of 2020 carries forward unabated, you will overstate the life expectancy declines it causes.
In effect, the CDC's assumption projects the impact of COVID-19 in a world in which none of the Operation Warp Speed vaccines exist seeing as they only began rolling out in large numbers in the latter half of December 2020.
When the CDC repeats its life expectancy exercise next year, its estimates of the change in life expectancy should reflect the first year impact of the new COVID-19 vaccines, which will make for an interesting side by side comparison. Especially when comparisons of pre-vaccine case and death rates with post-vaccine data already look like the New Stateman's chart for the United Kingdom:
Labels: coronavirus, health, risk, tool
What percentage of the population needs to be vaccinated to usefully reduce the risk of dying from COVID-19?
We're going to do a back-of-the-envelope calculation to estimate the answer to that question using Arizona's high quality COVID data in general, and the state's data for COVID-related hospital admissions and deaths in particular.
We're also going to build off our previous analysis that synchronized Arizona's figures for the number of positive COVID infection test results, hospitalizations, and deaths according to the approximate date of initial SARS-CoV-2 coronavirus exposure for the Arizonans who became infected and experienced these pandemic-related events. The following chart shows these three streams of data using a logarithmic scale, covering the period from 15 March 2020 through 30 April 2021.
We've annotated the chart to indicate two periods of "noise" in the data for deaths, which came into play when the daily number of COVID-related deaths of Arizonans dropped into the single digits. Because of the small numbers involved, having a relatively small change in the daily number can have an outsize effect on the appearance of the overall trend, which accounts for the "noisy" short-term trough that was recorded in mid-September 2020 and the short-term spike in late March 2021. We've added the dotted lines to these areas of the chart to indicate what the overall pattern would look like without the short term noise in the data.
Now to the bigger question. We're going to focus on the ratio of deaths to hospital admissions because these events represent the most serious classes of COVID infections. In Arizona, 75% of COVID-related deaths have occurred among the state's senior population, Age 65 or older. This same demographic has accounted for 46% of COVID-related hospital admissions in the state.
These figures confirm seniors are disproportionately vulnerable to both these outcomes if they become infected by the SARS-CoV-2 coronavirus. This fact is why this portion of the state's population was targeted for early COVID vaccinations once the vaccines became available.
Because the incidence of COVID-related deaths in concentrated in Arizona's senior population, we should see a sustained decline in the ratio of COVID deaths to hospital admissions corresponding to roughly when the population Age 65 or older achieved effective herd immunity. We can then identify what percentage of the state's elderly population had been received at least one vaccine dose at that point in time, which in turn, will give us a reasonable indication of what percentage of the population needs to be vaccinated for COVID to reduce its risk of death.
The next chart graphically shows the results when we combine these points of data together.
We find at least 55% of the population would need to have received at least one dose of the COVID-19 vaccines to provide the benefit of reduced risk of death from becoming infected by the coronavirus. That's the percentage of the Age 65 and older population of Arizonans who had been vaccinated as of 28 February 2021, which marks the point in time at which COVID-related deaths in the state began to plunge as a result of the Operation Warp Speed vaccination programs.
That's the low end for our estimate, because it does not consider the portion of the senior population who would have obtained natural immunity from having become infected with the SARS-CoV-2 coronavirus and who recovered from it. As of 28 February 2021, Arizona's senior population accounted for 109,897 known COVID infections, about 13.4% of the state's total at that time. Added to the 696,559 Age 65 or older Arizonans who had received at least one COVID vaccination dose at that date would put the high end of the estimate at 64%.
That upper level figure would explain why public health officials have set a target of 70% of the population for COVID vaccinations, but it seems strange they are not giving more weight to the potential contribution of natural immunity in achieving that goal. If they did, they could focus their limited resources for providing COVID vaccination more effectively.
Looking at Arizona's data, we would say the magic percentage for vaccinations to achieve useful COVID herd immunity is somewhere between 55% and 64% of the population. That's because there is almost certainly a good amount of overlap between those who have recovered from COVID and those who have been vaccinated. It would be more beneficial and less wasteful for public health officials to target the COVID vaccines to those who have not developed any antibodies to SARS-CoV-2 coronavirus infections.
References
Arizona Department of Health Services. COVID-19 Data Dashboard: Vaccine Administration. [Online Database]. Accessed 10 June 2021.
Labels: coronavirus, health, risk
Welcome to the blogosphere's toolchest! Here, unlike other blogs dedicated to analyzing current events, we create easy-to-use, simple tools to do the math related to them so you can get in on the action too! If you would like to learn more about these tools, or if you would like to contribute ideas to develop for this blog, please e-mail us at:
ironman at politicalcalculations
Thanks in advance!
Closing values for previous trading day.
This site is primarily powered by:
CSS Validation
RSS Site Feed
JavaScript
The tools on this site are built using JavaScript. If you would like to learn more, one of the best free resources on the web is available at W3Schools.com.